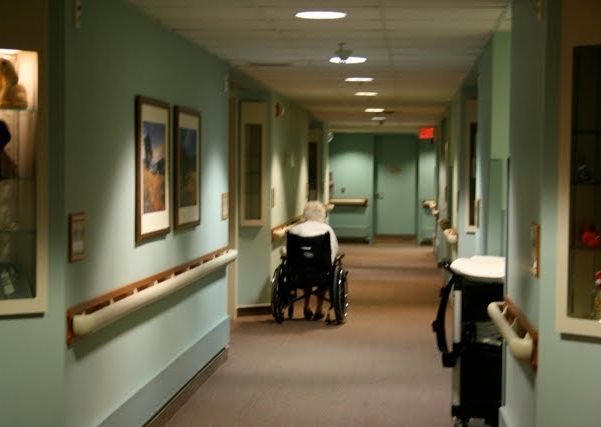
More are being attacked in long-term facilities
One day last June, staff at a Kamloops, B.C., nursing home found resident Jack Shippobotham, 79, lying on the floor with a broken nose, hip and pelvis.
He had wandered into the room of a fellow resident who, according to Shippobotham’s family, had a history of being “territorial.”
Shippobotham, who suffered from dementia, later told his family that “Big Foot had come down on his face.” Shippobotham made defensive motions with his arms to describe the attack, recalled his daughter, Moneca Jantzen.
Three weeks later, Shippobotham died of complications from his injuries, his family said.
Across Canada, reports of seniors being fatally attacked in care facilities, and dementia sufferers wandering away from nursing homes, have spurred calls to better track similar incidents, and to act on inquest recommendations that could prevent future tragedies among older, or mentally ill, people.
Susan Eng, vice-president of advocacy for the Canadian Association of Retired Persons, said she’s troubled by the spate of fatal attacks on residents at nursing homes by other residents, usually suffering from dementia.
“The nursing homes freely admit that they are not well-equipped to deal with the increasing incidence of mental illness among their intake population,” Eng told Postmedia News. “The specialized training has not been adequately funded and the regulatory requirements have not kept pace with the need.”
Eng wants a database created to track recommendations nationwide from inquests and inquiries probing the deaths of seniors.
Nursing homes need to be held to account when a tragedy occurs. But provinces also need to conduct systemic reviews, either by reviewing all or a random set of deaths in nursing homes, she argued.
This article was published by the Calgary Herald on January 22nd, 2014. To see this article and other related articles on their website, click here.
Shippobotham’s alleged assailant, a 71-year-old resident, later died. Shippobotham’s daughter still has questions, such as whether improved security at the Overlander Residential Care facility might have prevented the attack.
“I think we also need to look at how we’re ‘warehousing’ our elders,” Jantzen said in an email to Postmedia News. “Do we have enough staff and with the right combination of skills and qualifications? Placement of people is critical so assessments need to be completed. And if and when someone changes and becomes violent, they need to have a reasonable solution for that.”
Just weeks after that incident, William May, an 85-yearold resident at the Polson Residential Care facility in Vernon, B.C., died after allegedly being assaulted by his 94-year-old roommate. The roommate, John Furman, was charged with second-degree murder, but the Crown stayed the charge because of Furman’s advanced dementia.
Both cases are now being reviewed to see if they warrant an inquest or deeper examination by a death-review panel, says the British Columbia Coroners Service.
A pair of attacks in the Toronto area last year triggered similar alarms.
Francisco DaSilva, 87, was found dead at the Castleview Wychwood Towers nursing home in November with “obvious injuries to the head,” police said. His roommate, 81-year-old Francesco Greco, was charged with second-degree murder.
Earlier, 72-year-old Joycelyn Dickson was found dead at the Wexford Residence long-term care facility in March, allegedly beaten with a cane. Another resident, 72-year-old Peter Brooks, was charged with second-degree murder.
The homicides prompted the Ontario Nurses’ Association to call on the province to act on key recommendations from a previous inquest – held in 2005 into the deaths of two residents at the Casa Verde nursing home in Toronto.
Piara Singh Sandhu, 74, had been at the facility less than a day when he used a piece of metal to attack Ezz-El-Dine El-Roubi, 71, and Pedro Lopez, 83. Sandhu, who suffered from dementia and had a history of aggression, was charged with two counts of second-degree murder but died in custody.
An inquest jury delivered 85 recommendations. It said the province should give “increased priority” to ensuring nursing homes have proper funding and standards to manage residents with cognitive impairments; that people who are considered a risk to themselves or others should not be admitted into any facility until they have been assessed and a care plan developed; and that the province should create specialized facilities and units to care for residents with behavioural problems.
Citing the Sandhu case, Ontario’s geriatric and long-termcare review committee warned in a 2011 report that as a result of Canada’s aging population, long-term-care homes were becoming the new “mental health institutions.”
“Safety of current and future residents will continue to be at risk without the appropriate and prompt development of comprehensive plans and protocols for the management” of dementia sufferers, the report said.
It’s expected more than 1.4 million Canadians will have dementia by 2031, up from 750,000 today. The Canadian Medical Association last year called for a national strategy on dementia.
Meanwhile, advocates are also calling attention to the growing problem of seniors who simply wander away from care homes.
Last month, the body of 76-year-old Joan Warren was found by a hiker in the Lynn Canyon area of North Vancouver. She had walked away from the Sunrise of Lynn Valley long-term-care facility in sub-zero temperatures.
A similar incident several years ago in Alberta prompted a fatality inquiry, but many of the recommendations have not been acted on. On the morning of Dec. 31, 2007, staffat The View Holiday Retirement Home in Lethbridge, Alta., noticed that 88-yearold resident Sydney Salter was missing at breakfast. His body was discovered in the parking lot about 100 yards away from the facility, and was covered by a small amount of fresh snow.
Salter, who suffered from dementia and had a history of wandering at night, was barefoot and dressed only in light pants and a shirt. It was -15 C that morning.
After a two-day fatality inquiry, provincial Judge Ronald Jacobson recommended in September 2009 that the province’s health ministry bring together health professionals, health-care providers and other experts for an independent study to determine the best short-and long-term care for people with dementia, Alzheimer’s and other “cognitive impairments.” The study, the judge said, should examine the needs of “wanderers” and the use of GPS-monitoring devices.
The study should also review communications systems to ensure that whenever a marked change occurs in a patient’s health, all health-care providers and family members are notified immediately.
Signalling the urgency of the matter, the judge recommended that findings be published by Jan. 31, 2010.
Haydon Dewes, a spokesman for Alberta Health Services, said a study was conducted but it was an “internal report” and not published. He could not say why the study was not published.
At the time the judge’s report came out, health officials said the province was working on a “dementia strategy.” Four years later, the strategy is still being developed.
“Have we developed a provincial dementia strategy? No, we have not,” said Brenda Huband, interim CEO of clinical operations for Alberta Health Services. But Huband said the province has introduced a number of measures that are “well-aligned” with concerns raised at the inquiry and that will eventually form part of a dementia strategy.
After assessing the ethical implications, early this year Alberta Health Services will roll out pilot tests of locator technology on patients at risk of wandering.
Health officials are also working with dementia-care experts on ways to reduce the use of anti-psychotic medications, which can have serious side-effects.
The province has also been providing specialty training to continuing-care and acute care staff for dealing with dementia patients.
Ruth Adria, spokeswoman for Elder Advocates of Alberta Society, said while fatality inquiries in Alberta have done a good job of exposing problems in elder care, the province has done a “very poor” job of following up on recommendations.
“The whole process is just posturing. As soon as it finishes, there’s no consideration given” to recommendations, she said. “We have very little confidence in the system.”
Dying to be heard
About this series: Postmedia News reporter Douglas Quan spoke with experts, advocates and families about the problems plaguing Canada’s ailing inquest system. See his full series, with video, at calgaryherald.com/inquests Saturday: Why the findings of inquests and fatality inquiries often go unheeded.
Monday: Probing the police: Inquests and incustody deaths. Tuesday: What governments can learn from inquiries into child fatalities. Wednesday: Plight of seniors in care begs better followup.
Thursday: Should inquests be mandatory for all workplace deaths? Friday: How inquests can be made more effective.